Sports from the neck up: Coquitlam Express chart a course for brain health in the concussion era
New tech could allow an athletic therapist to see how a hockey player’s brain is functioning following a big hit

There’s something down the hall that maybe – just maybe – could change hockey for the better.
I’m in the Surrey Neuroplasticity Clinic just off King George Boulevard. The clinic, located in the health and technology hub just north of Surrey Memorial Hospital, is set to be an important stop for the Coquitlam Express hockey club next season, following the team’s announcement of a partnership with the clinic earlier this spring.
As I head down the hall, the clinic’s marketing and business development manager Balraj Dhillon braces me for what I’m about to see.
It’s patented, he tells me.
Local news that matters to you
No one covers the Tri-Cities like we do. But we need your help to keep our community journalism sustainable.
It’s proprietary, I learn.
I turn down the hall, thinking of every hockey player who went back on the ice after he had his “bell rung” and paid a terrible price in chronic brain trauma. And then I see what appears to be a shower cap with delusions of grandeur.
It’s called The NeuroCatch.
With red wires, electrodes, and a chin strap that makes you feel like an old-timey fighter pilot, it’s somewhat reminiscent of the telepathy machine Doc Brown stuck on Marty’s head in Back to the Future.
The NeuoCatch, despite its humble appearance, represents an idea that used to be strictly science fiction: it’s a look at the inner workings of your mind.
There are no questions to answer or activities to complete.
Tones sound in the patient’s ears as they stare at a cross on the wall. Clinicians track the ensuing electrical signals produced by the brain, mapping rises and dips in order to: “detect subtle neurophysiological presentations of brain injury.”
They used “oddball tone stimuli” as well as word pairs. The idea is that your brain reacts one way to “bread-butter,” and completely differently to “bread-window.”
The brain reacts to each stimuli and the speed of those reactions is measured in milliseconds.
As a demonstration, kinesiologist Mathieu Gagnon shows the results produced by a patient who suffered a head injury.
By contrasting the new results with a baseline, you can see where reaction time falls like Bitcoin stock.
Almost every other test for brain health requires some sort of performance or self-reporting. This test is “non-fungible,” says Gagnon, a Coquitlam resident.
The plan is to test players in the preseason and keep track of “all those little traumas,” Dhillon says.
Asked if athletes might be hesitant to have their brain activity monitored, Gagnon says a lot of athletes are curious about using the technology to see how their brains are doing.
“It’s part of being on a team,” Dhillon says. “No one’s going to end their junior hockey career because they don’t want their brains scanned.”
The NeuroCatch evaluation takes about six minutes. Corresponding data is produced immediately.
Doctors would still have the final say on whether a player can get back on the ice or not. But, after years of judging how a player looks and how a player sounds, this is the first attempt to understand how a player thinks.

Hard data for tough calls
Generally, the decision to put a player on the ice or the bench comes down to what you can observe and what the player is willing to report, explains Gaëlle Bergeron, the new athletic therapist for the Coquitlam Express.
“If the athlete isn’t truthful it’s very hard to get reliable information,” she says. “Having hard data that comes from a computer and from brain activity is definitely a big improvement and a big step up.”
In addition to being an athletic therapist and equipment manager, Bergeron says she often serves as “relationship counsellor, mom, friend, [and] big sister,” for her players.
That closeness has helped her do her job, she says, explaining that she can often tell the difference from a player who says he’s fine and a player who really is.
“I try to get to a point where players are comfortable enough with me that they trust me with – not just their hockey issues, but personal issues,” she says. “Their safety and physical and mental well-being is put at the top of our priorities and not just winning at all costs.”
The players are set to head to the neuroplasticity clinic in August. The clinic’s process, which forms a baseline for each player’s brain, balance and cognitive abilities, is set to take about four hours per player, Bergeron says. Previously, a similar intake took about 10 to 15 minutes per athlete, she notes.
“We’ll figure out a schedule that works.”
The work the clinic is doing rests, in part, on work led by neuroscientist Dr. Ryan D’Arcy.
Your brain on hockey
Over two seasons, D’Arcy watched teens and young adults play hockey with sensors attached to their helmets.
The idea was to find out how often kids were getting hit in the head and what those hits were doing to their brains.
While there’s been an emphasis on The Big Hit in research, this study focused on “sub-concussive impacts.”
“The effects of these low-magnitude impacts may not even be noticeable to the player or to observers on the sideline,” the study notes. “However, it has been shown that repetitive sub-concussive impacts over time can result in structural and functional brain impairment.”
The study concluded that changes to brain function were “significantly correlated” with the number of impacts to the head.
That conclusion can be off-putting, D’Arcy notes.
“I think that most people’s first reaction is: ‘That’s frightening. . . . Are you telling me that physical games like hockey shouldn’t be played?’ . . . That’s not the case,” he says. “What we’re telling you is, we can manage it now and we can find ways to treat it.”
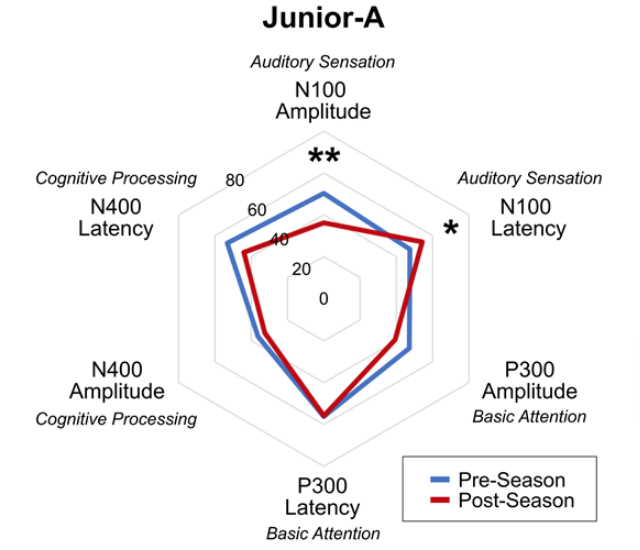
Research in the Express lane
The brain-body program’s ambition is to test something that has long been an abstract concept in sports: presence of mind.
It’s about “cognitive agility,” D’Arcy explains.
D’Arcy likens the human brain to a supercomputer. “That supercomputer needs to process information and you want it to process as quickly as possible.”
This program, D’Arcy says, is like slapping a speedometer on your mind’s processing speed.
“Anything that affects that, we will detect,” he says, noting that brain function could be impacted by poor sleep or a cup of coffee.
“It’s really unique that it’s brain and body together because we tend to think of those as being separate,” he says.
A fundamental part of the program is balance, he says.
“If we actually improve your balance, we can improve your cognition,” he says. “The reverse is likely true as well.”
To that end, the first stop at the Surrey Neuroplasticity Clinic looks like an unfinished elevator.
It’s an “objective measure of balance,” Gagnon explains as he walks to the Neurocom balance monitor.
After being strapped into a harness, the patient adjusts to stay upright as the floor rises and tilts.
Besides checking to see if the patient is balancing, the machine is designed to detect exactly how a patient is balancing and whether they’re relying on their muscles, eyes or inner ear.
It’s important to monitor which tools an athlete is using, particularly following an injury, Gagnon explains.
Generally speaking, an injured athlete tends to be a chameleon, compensating to disguise and overcome whatever isn’t working.
“We’re not making a medical decision based on your subjective reporting . . . you literally can’t balance,” Dhillon explains.
The balance board is tough to beat.
“We move the walls, we move the floor,” Gagnon says, noting the patient’s score is calculated by a computer algorithm. “It can’t really be fudged that much.”